Lecture Note
Unit 11 Review
-
University:
University of Alberta -
Course:
NURS 106 | Foundations of Anatomy and Physiology for Nursing Academic year:
2024
-
Views:
302
Pages:
3
Author:
Ali O
Related Documents
- Seven Levels of Listening
- Silent Message and Bon Verbal Listening Test
- Laws of Remembering
- Relevant Oast Histories of a Patient
- Laws of Forgetting
- Hearing of Words and Communication Circle
- Anatomical Structures in Hip Joint
- Attention Spans Class Notes
- GFR Calculation Course Materials
- Chronic Inflammation of Tubulo Interstitial Tissues
- Femoral Traingle and Popliteal Fossa
- Importance of Psychology in Physiotherapy
- Gingival Calculi
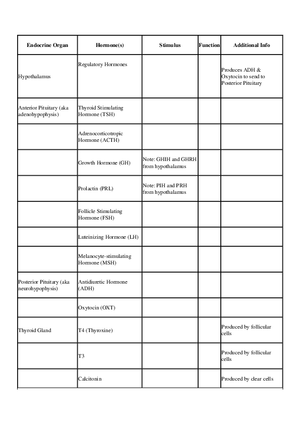
- Biosynthesis of Thyroid
- GI Tract and JG Apparatus
- Manual Muscle Test and Gait
- Case History and General Physical Examination
- Patient Examinations
- X-ray Device - Study Note
- Pulpal Disease
Report
Tell us what’s wrong with it:
Thanks, got it!
We will moderate it soon!
Report
Tell us what’s wrong with it:
Free up your schedule!
Our EduBirdie Experts Are Here for You 24/7! Just fill out a form and let us know how we can assist you.
Take 5 seconds to unlock
Enter your email below and get instant access to your document